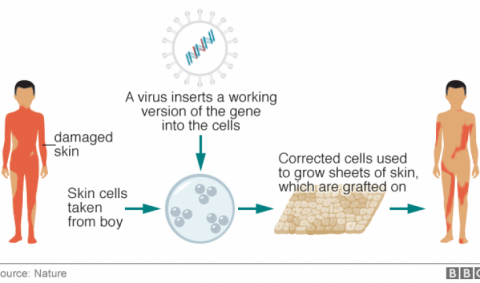
Regeneration of the entire human skin using transgenic stem cells
Prof Michele De Luca, from the University of Modena and Reggio Emilia, told the BBC: “The gene is different, the protein is different and the outcome may be different [for each form of EB] so we need formal clinical trials.” But if they can make it work, it could be a therapy that lasts a lifetime. An analysis of the structure of the skin of the first patient to get 80% of his replaced has discovered a group of long-lived stem cells are that constantly renewing his genetically modified skin.
– Genetically modified skin cells were grown to make skin grafts totalling 0.85 sq m (9 sq ft).
– It took three operations over that winter to cover 80% of the child’s body in the new skin.
– But 21 months later, the skin is functioning normally with no sign of blistering.
Junctional epidermolysis bullosa (JEB) is a severe and often lethal genetic disease caused by mutations in genes encoding the basement membrane component laminin-332. Surviving patients with JEB develop chronic wounds to the skin and mucosa, which impair their quality of life and lead to skin cancer. Here we show that autologous transgenic keratinocyte cultures regenerated an entire, fully functional epidermis on a seven-year-old child suffering from a devastating, life-threatening form of JEB. The proviral integration pattern was maintained in vivo and epidermal renewal did not cause any clonal selection. Clonal tracing showed that the human epidermis is sustained not by equipotent progenitors, but by a limited number of long-lived stem cells, detected as holoclones, that can extensively self-renew in vitro and in vivo and produce progenitors that replenish terminally differentiated keratinocytes. This study provides a blueprint that can be applied to other stem cell-mediated combined ex vivo cell and gene therapies.